ELETTRA REPETTO
This year it is the 40th anniversary of the CDC Morbidity and Mortality Weekly Report, the first medical document that recognized the disease later known as AIDS. So, this World AIDS Day, to remember this important discovery and look ahead, I discussed HIV with Maria Viscoli of Anlaids, the Italian Association for HIV prevention.
A name, a diagnosis
First of all, what is AIDS? AIDS – acquired immunodeficiency syndrome – is a disease attacking the immune system and rendering people susceptible to other illnesses and conditions, such as Tuberculosis and Pneumonia. AIDS is caused by the infection with HIV – human immunodeficiency virus. HIV is spread primarily by unprotected sex (including anal and oral sex), contaminated blood transfusions, hypodermic needles, and from mother to child during pregnancy, delivery, or breastfeeding. Saliva, sharing food or drinks, insects do not transmit the virus, as it was mistakenly believed in the past.
What changed these four decades?
From its 1981 discovery, a lot of things have improved as it is evident by looking at the data showing infections and deaths around the world. This is true for all the world and communities notwithstanding the differences in access to treatments and prevention services.
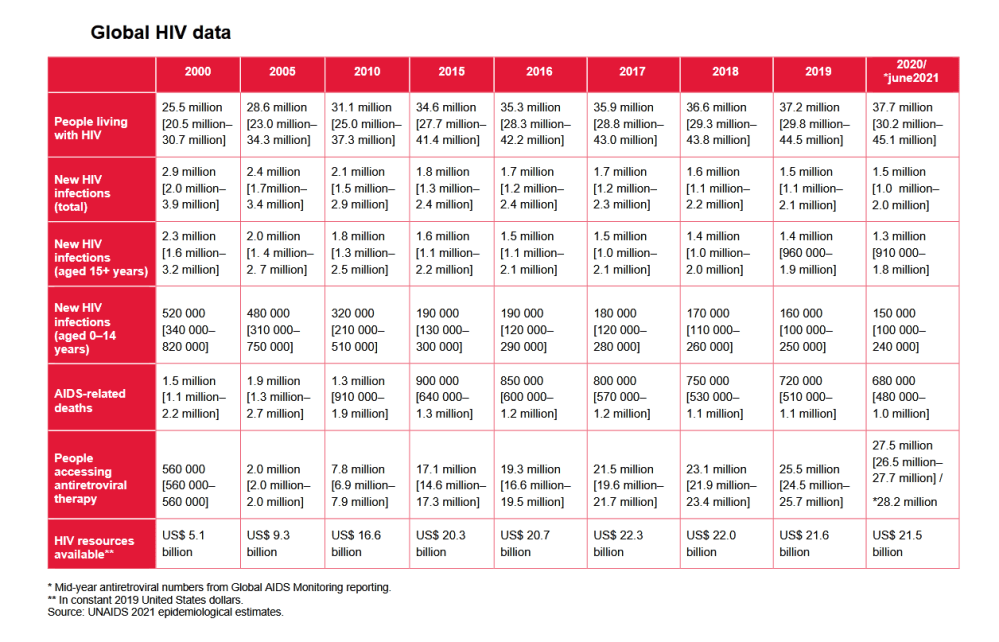
Thanks to antiretroviral therapies many HIV-positive people can now lead a life like anyone else, have a family, and even diminish their viral charge to the point of not being contagious anymore. As for their life expectancy, people who receive an early diagnosis and are following their treatments can live a life as long as people who are not HIV-positive. This was quite unheard of just a few decades ago. In 40 years we have passed from naming the disease to immensely advance in curing it.
The introduction of PrEP has also been quite a life-changing innovation, although the number of people taking it is still below the UNAIDS target of 3 million. PrEP stands for Pre-Exposure Prophylaxis and comes in the form of a pill that prevents people from getting AIDS by about 40- 90% depending on whether people take it as prescribed.
Worth mentioning is also the decreasing infections among infants. While in the past it was common to have newborns suffering from AIDS, HIV-positive women in many parts of the world can now give birth to a healthy child. For instance, in Italy, says Maria Viscoli, “it has been years since last HIV-positive infant was born”.
COVID19 & AIDS
While things have been improving, the pandemic has put numerous activities related to HIV prevention and treatment on hold. HIV-positive people are indeed dependent on daily medications that during the pandemic were difficult to find given the closure of borders in richer countries, and impossible to find in poorer ones. The hospitals, already overwhelmed with COVID patients, delayed or canceled the check-ups, local associations did not organize tests and information services as before. Mental health services were stopped, or were only partially open. Those that kept their check-points open were normally doing so under appointment and asking for registration, with a view to tracking people in case of a COVID outburst, which meant the complete loss of the fundamental privacy guarantees, dissuading people to get tested.
All of this led to delays in getting an early diagnosis, says Viscoli, with consequences that we will discover only in the coming years. Indeed, although the current UNAIDS data talks about 79.3 million people becoming infected with HIV and 36.3 million people dying from AIDS-related illnesses since the start of the epidemic, these data do not help us to predict the future trend.
As for the number of deaths and hospitalization: HIV positive individuals were and are more at risk to get COVID and get seriously sick, and since they could not access testing and prevention cures, they might have seen their illness progress before they could even know they were infected and could act on it. This is especially grave for people in Africa where COVID-19 vaccines are scarce and people are more at risk of contracting both COVID and HIV.
Globally, according to the Global Fund “people reached with HIV prevention programs and services declined by 11% while young people reached with prevention services declined by 12%. Mothers receiving medicine to prevent transmitting HIV to their babies dropped by 4.5%. HIV testing dropped by 22%, holding back HIV treatment initiation in most countries”.
In some regions of the world, HIV-positive individuals were blamed to be the carrier of COVID-19, while access to justice was limited and discrimination went up. Given this persisting stigma surrounding HIV/AIDS, it is not surprising then that a lot of people tend to get cured far from home, travelling to do their check-ups and relying on HIV centers in different cities. “In Italy, a person living in a certain area may go to another area to get cured, to maintain her privacy and be sure to not meet anyone she might know. During the pandemic, travelling across regions was not permitted and this became a problem for many, who had to reorganize their medical routine and ask for assistance closer home” – confides Viscoli.
Sadly, but not surprisingly, things became even harder in poorer areas. In Africa, where the highest percentage of HIV-positive people reside, many did not receive the medication that in normal times would have been shipped there, but now never arrived. In addition to this, there was also a lack of trained personnel, including doctors and nurses.
The pandemic, moreover, also led to economic consequences that directly affected the possibility to engage in HIV prevention. If in the past a lot of associations could safely rely on private donations coming from medical corporations and private citizens, this year most of the funds were dedicated to COVID tests and cures.
The Way Forward
Today, forty years after the publication of the CDC report, HIV is still a serious illness and yet remains a silent one. Although many countries have in place mechanisms to address HIV-related discrimination, there is a disturbing lingering cultural stigma attached to HIV/AIDS that is strong to the point that many avoid testing and delay seeking treatments.
Also, evident ethnic-based disparities exist in access to tests and cures that need to be addressed. If we look at the 2019 US Centers for Disease and Prevention data we see that just 8% of black Americans and 14% of Hispanics/Latinos who were eligible for pre-exposure prophylaxis (PrEP) were prescribed it, compared to 63% of whites. In addition, PrEP is not free of charge. In Italy, a monthly treatment costs 60 euro, in the US around 1600 US dollars without health insurance. If this might not be a problem for many, this could still impede some to get it.
“In Italy a monthly treatment costs 60 euro, in the US around 1600 US dollars without health insurance”
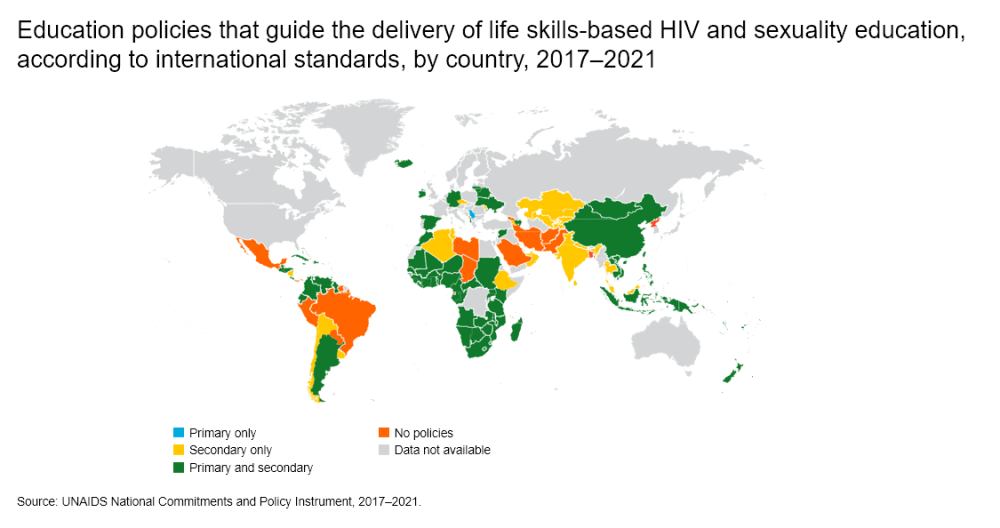
Moreover, prevention passes also, and most importantly, through education which is lacking everywhere, for different reasons. The countries where there are sex-ed classes are few and those that have them do not necessarily follow a precise curriculum while teaching kids to use condoms and get tested is essential.
“In Italy, it all depends on the goodwill of the professors. We have established good relationships with some who contact us and ask us to talk about HIV/AIDS to kids, but access is never for granted. In the beginning, it was very hard for us to educate kids because schools simply did not call us and such education is not compulsory” says Viscoli.
Also, Viscoli adds, “according to a 1990 law, if you are under 18 you cannot get tested in Italy without the consent of your parents. This means sexually active adolescents may never get tested, contract the virus and spread it without knowing it”. Testing is essential to protect us and the ones we meet, and the sooner it is done, the better. This is why Anlaids is involved in a plan to revise the 1990 Italian law on HIV prevention and adaptation to finally allow minors to act autonomously in safeguarding their health and, this way, to actively combat discrimination.
Sex and health education have to be part of school education everywhere, condoms need to be free in schools and tests need to be easy to do. This does not simply require “a safe environment protecting anonymity and guaranteeing confidentiality, but also centers opened beyond working hours and during the weekends, to avoid people from having to justify their request for a day or a morning off”, explains Viscoli, who has just helped open the latest Anlaids checkpoint in Italy.
Safe-sex and safe drug use, combined with regular tests and proper medications in case of infection are essential to lower the number of yearly cases and improve the lives of those who turn out to be HIV-positive. All of this would directly enhance HIV-positive people’s lives and their families’ but all of ours, as well. If COVID taught us one thing, it is that we are related to each other more than we thought and whatever happens to you might happen to me. We have to care for each other, protect ourselves so as to protect others, but also avoid discriminating against people. We have achieved a lot these past 40 years, who knows what we can do in the decades to come.



























